Our Blog
Abfraction Restorations
Over time we find they can fracture or discolor.
How do I prevent that?
After 25 years of dentistry I’ve made some observations and modifications to techniques. Addition of instrumentation such as diode and then hard tissue lasers have changed how we complete these restorations. The Waterlase iPlus has been a very effective tool and the most recent version of the software even lays out the steps for restorative. Many times the gingiva has grown up to and maybe even over what cavosurface margin would exist. The body is trying to heal and protect itself. The abfraction lesion can be sensitive to cold, touch and if allowed to continue growing will become a problem to the central nerve of the tooth.

Preparation
Years ago we would cut the gum tissue back and allow it to heal. Then upon return we would pack cord into the sulcus of the gum to push it back. A successful restoration would need to be placed in the absence of sulcus crevicular fluid and or blood. To do this “correctly” it would be a multi visit and time consuming process.
When I adopted a diode laser we could cut the gum tissue back to its correct position and if the gum tissue was stable and healthy we could restore in a bloodless, dry environment.
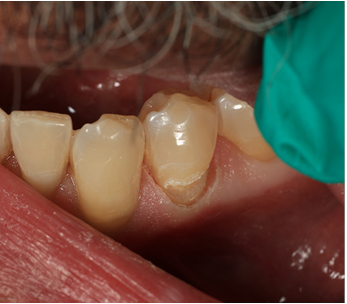
I added another laser which is a hard and soft tissue laser. Waterlase iPlus Premium. (of course any laser that has hard and soft or just soft tissue function will suffice. This just happens to be my choice) this laser allows me to trim to soft tissue and create a sulcus that will not leak and then immediately follow with hard tissue preparation. That preparation follows the same old rules of creating a squared off ledge that can give us mechanical retention. I do take my diamond and bevel the occlusal most portion so that the composite will feather into the original tooth structure and it becomes more difficult to detect a color change.
The root surface is a very porous one. The patient can already be sensitive in this location and acid etching, while necessary, can make that sensitivity worse. At times the patient would be improved and at times the patient would find that the sensitivity would linger.
My bonding process has thus evolved. I still need to bond to the tooth and so still need to etch the dentin. I want to limit sensitivity so I use XTR by the Kerr Corp. The research shows that the bond strength to dentin was very high. But a little lower on enamel than my previous. Over months I would find a thin brown line at the enamel junction. To solve this….i phosphoric acid etch just that enamel margin. Air abrasion at the enamel margin. And finally bonding agent - XTR by Kerr is a two step etch liquid and bond liquid. The primer liquid is self etch and whatever it touches it etches but also helps to seal. In this way it reduces post op sensitivity (by not over etching onto unbonded surfaces). To bond to the dentin and enamel the above method alone is perfectly adequate. But if I want to increase bond strength of the XTR to enamel I will spot etch the enamel at the occlusal most portion of my preparation. I also air etch the enamel only.
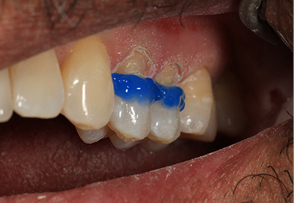
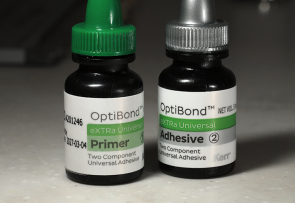
I have been doing this for the past 10 years or so we do not find staining of any margin due to bonding weakness or leakage. I have also found that the sensitivity post op has dropped to maybe 1 in 10. And maybe 1 in a 100 might have lingering sensitivity.
Restoration
There are multiple considerations with Abfraction lesions. We have gingiva, dentin and enamel. Specifically the dentin on the root is sensitive to acids. Our procedures can sensitize the area and the neighboring areas.
Over the years I have modified my chemical preparation of the root surface as well.
Firstly the restorative material must be flexible. It cannot be a packable rigid material. The cause of the abfraction is flexure of the underlying flexible dentin root. As the attached enamel is very thin at the CEJ it will eventually crack. The forces at the CEJ continue to cause flexure and increase the size of the abfraction lesion. So restoration must have a flexible lightly filled restorative material. If the material is too highly filled or is inflexible it will break away just like the original tooth did.
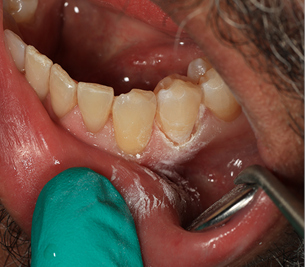
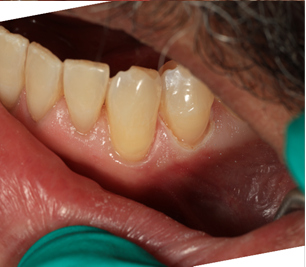
For about 20 years I have specifically use a Japanese manufactured material TMPT by Parkell corp. it survives very well resists staining. It is easy to sculpt and in this location is easier to manipulate.
For this I have one final step. After contouring and polishing. We take Enamelon by Premier prophy paste. It is an Amorphous Calcium Phosphate paste. Prophy cup application to the CEJ and surrounding root area will drop sensitivity by occluding any remaining open pores. Remember open pores at the root are odontoblast canals and they channel right back to the central nerve of the tooth. The restoration covers this but if some are open the sensitivity can remain. The saliva has calcium and this is why time can correct the sensitivity but adding this at the time when the patient is already numb is important.

Cover the area immediately after with a sticky paint on fluoride and my sensitivity is much much less. Most patients do not think about the tooth again. Of course there will always be a tooth that is sensitive and defies all these efforts but with this method has been tried and true for the past 10 plus years. In fact we recently replaced a restoration that broke and we realized that it had been 12 years since I placed it. In hindsight there are only a handful of these that have even needed to be replaced.
